Nightly Phenomena, Day Time Work?
R. Tukkie, R. Rienks, A.A.M. Wilde
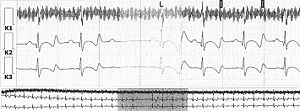
In 2002, an a trial demand inhibited (AAI) pacemaker was implanted in a young male (born 1984) because of a primary arrhythmia disorder. On a routine Holter recording, the following rhythm strip was recorded
Early in the morning during sleep (figure 1).
Which phenomenon is visible?
The rhythm strip shows an atrial paced rhythm with conduction to the ventricle in the first two beats. The third atrial paced beat is not conducted to the ventricle because of a second-degree AV block Wenckebach type. The P-R interval increases from the first to the second beat and the P-R interval of the beat after the pause shortens again. The Wenckebach block is promoted by the relatively high lower rate programmed in this patient of 60 bpm.
Which primary electrical disease is present?
The ST segments are clearly abnormally shaped (biphasic) with also marked QT prolongation present (QTc 560 ms). The diagnosis is long-QT syndrome (LQTS). In this patient and other family members a sodium channel mutation was found (in the SCN5A gene) proving the diagnosis LQTS type III. These patients suffer from an increased risk of nocturnal sudden death.1,2 Adrenergic blockade is known to be not very effective in preventing SCD in these patients. The torsades de pointes in LQTS type III are bradycardia dependent. In this specific family, atrial pacing is known to prevent sudden cardiac death but in other patients ICD therapy may be indicated.3 Optimal pacing should prevent bradycardia and pauses. AV search hysteresis and night drop responses should be programmed off.
What is the consequence of the observed phenomenon in question 1 in the setting of this patient’s primary electrical disease?
As a result of the pause after the non-conducted atrial paced beat, the QT interval further prolongs significantly to QTc 740 ms, increasing the risk of torsades de pointes. QT prolongation at bradycardia is a feature of
type III LQTS.
What action should be undertaken?
It is mandatory to prevent relative bradycardia and pauses due to Wenckebach block in this patient. This can be achieved by adding a ventricular lead and programming the new pacemaker to duel-chamber with an AV delay long enough to advocate intrinsic AV conduction to the ventricle. Our patient underwent an uneventful upgrade and a control Holter recording showed excellent prevention of pauses.