Myocardial Infarction
| Author(s) | I.A.C. van der Bilt, MD | |
| Moderator | I.A.C. van der Bilt, MD | |
| Supervisor | ||
| some notes about authorship | ||
Ischemia occurs when part of the heartmuscle, the myocardium, is deprived form oxygen and nutrients. Common causes of ischemia are:
- Narrowing or obstruction of a coronary artery.
- A rapid arrhythmia, causing a disbalance in supply and demand of energy.
A short period of ischemia causes reversible effects: The heartcells will be able to recover. When the episode of ischemia lasts for a longer period of time, heartmuscle cells will die. This is called a heart attack or myocardial infarction. That is why it is critical to recognize ischemia on the ECG in an early stage.
Severe ischemia results in ECG changes within minutes. While the ischemia lasts, several ECG changes will occur and disappear again. Therefore, it may be difficult to estimate the duration of the ischemia on the ECG, which is crucial for adequate treatment.
Signs and symptoms of myocardial ischemia:
- Crushing pain on the chest (angina pectoris), behind the sternum, often radiating to the lower jaw or the left arm
- Fear of dying
- Nausea
- Shock (manifesting as paleness, low blood pressure, fast weak pulse) shock
- Rhythm dysturbances (in particular increasing prevalnce of ventricular ectopia, ventricular tachycardia, AV block)
Risk assessment of Cardiovascular disease
The narrowing of the coronary artery leading to a myocardial infarction, usually develops over several years. An increased risk of cardiovascular disease, which may lead to a myocardial infarction or stroke, can be estimated using SCORE system which is developed by the European Society of cardiology (ESC). As shown in the figure, the most important risk factors for myocardial infarction are:
- Male sex
- Smoking
- Hypertension
- Diabetes Mellitus
- Hypercholesterolemia
Risk assessment of ischemia
An exercise test such as a bicycle or treadmilltest, may be usefull in detecting myocardial ischemia after exercise.[1] In such a test, a continuous ECG registration is performed during exercise. The ST-segment, blood pressure asnd clinical status of the patient (i.e. chest complaints) are monitorered during and after the test.
An exercise test is positive for myocardial ischemia when the following criteria are met:
- Horizontal or downsloping ST-depression of > 1mm, 60 or 80ms after the J-point
- ST elevation of > 1.0 mm
Diagnosis of myocardial infarction
The diagnosis of acute myocardial infarction is not only based on the ECG. A myocardial infarction is defined as:[2]
- Elevated blood levels of cardiac enzymes (CKMB or Troponin T) AND
- One of the following criteria are met:
- The patient has typical complaints
- The ECG shows ST elevation or depression
- pathological Q waves develop on the ECG
- A coronary intervention had been performed (such as stent placement)
So detection of elevated serum heartenzymes is more important than ECG changes. However, the heartenzymes can only be detected in the serum 5-7 hours after the onset of the myocardial infarction. So especially in the first few hours after the myocardial infarction the ECG can be crucial.
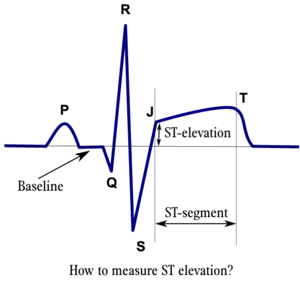
- Significant ST elevation is defined as
- ST elevation of more than 2mm in two chest leads or more than 1 mm in two adjacent limb leads
- ST elevation is measured 60ms or 80ms after the J-point
A study using MRI to diagnose myocardial infarction has shown that more emphasis on ST depression could greatly improve the yield of the ECG in the diagnosis of myocardial infarction (sensitivity increase from 50% to 84%).[3]
Myocardial infarction diagnosis in left or right bundle branch block can be difficult, but is explained in these seperate chapters:
The location of the infarct
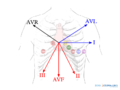
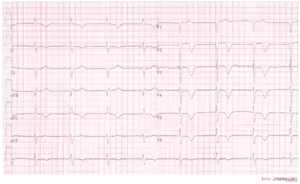
Overview of the seperate ECG leads. The lead with ST elevation 'highlights' the infarct. An infarction of the inferior wall will result in ST elevation in leads II, III and AVF. A lateral wall infarct results in ST elevation in leads I and AVL. An Anterior wall infarct results in ST-elevation in the precordial leads.
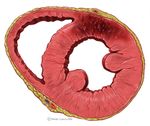
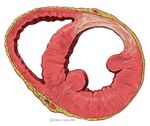
The heartmuscle itself is very limited in its capacity to extract oxygen in the blood that is being pumped. Only the inner layers (the endocardium) profit from this oxygenrich blood. The outer layers of the heart (the epicardium) are dependent on the coronary arteries for the supply of oxygen and nutrients. With aid of an ECG, the occluded coronary can be identified. This is valuable information for the clinician, because treatment and complications of for instance an anterior wall infarction is different than those of an inferior wall infarction. The anterior wall performs the main pump function, and decay of the function of this wall will lead to decrease of bloodpressure, increase of heartrate, shock and on a longer term: heart failure. An inferior wall infarction is often accompanied with a decrease in heartrate because of involvement of the sinusnode. Longterm effects of an inferior wall infarction are usually less severe than those of an anterior wall infarction.
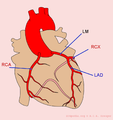
The heart is supplied of oxygen and nutrients by the right and left coronary arteries. The left coronary artery (the Left Main or LM) divides itself in the left anterior descending artery (LAD) and the ramus circumflexus (RCX). The right coronary artery (RCA) connects to the ramus descendens posterior (RDP). With 20% of the normal population the RDP is supplied by the RCX. This called left dominance.
Below you can find several different types of myocardial infarcation. Click on the specific infarct location to see examples.
| localisation | ST elevation | Reciproke ST depression | coronary artery |
|---|---|---|---|
| Anterior MI | V1-V6 | None | LAD |
| Septal MI | V1-V4, disappearance of septum Q in leads V5,V6 | none | LAD |
| Lateral MI | I, aVL, V5, V6 | II,III, aVF | RCX or MO |
| Inferior MI | II, III, aVF | I, aVL | RCA (80%) or RCX (20%) |
| Posterior MI | V7, V8, V9 | high R in V1-V3 with ST depression V1-V3 > 2mm (mirror view) | RCX |
| Right Ventricle MI | V1, V4R | I, aVL | RCA |
| Atrial MI | PTa in I,V5,V6 | PTa in I,II, or III | RCA |
The localisation of the occlusion can be adequately visualized using a coronary angiogram (CAG). On the CAG report, the place of the occlusion is often graded with a number (for example LAD(7)) using the classification of the American Heart Association.[4]
Development of the ECG during persistent ischemia
The cardiomyocytes in the subendocardial layers are especcially vulnerable for a decreased perfusion. Subendocardial ischemia manifests as ST depression and is usually reversible. In a myocardial infarction transmural ischemia develops.
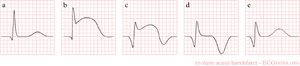
In the first hours and days after the onset of a myocardial infarction, several changes can be observed on the ECG. First, large peaked T waves (or hyperacute T waves), then ST elevation, then negative T waves and finally pathologic Q waves develop.
| Time from onset of symptoms | ECG | Changes in the heart |
|---|---|---|
| minutes | hyperacute T waves (tall T waves), ST-elevation | reversible ischemic damage |
| hours | ST-elevation, with terminal negative T waves, negative T waves (these can last for days to months) | onset of myocardial necrosis |
| days | Pathologic Q Waves | scar formation |
References
- Gibbons RJ, Balady GJ, Bricker JT, Chaitman BR, Fletcher GF, Froelicher VF, Mark DB, McCallister BD, Mooss AN, O'Reilly MG, Winters WL Jr, Gibbons RJ, Antman EM, Alpert JS, Faxon DP, Fuster V, Gregoratos G, Hiratzka LF, Jacobs AK, Russell RO, Smith SC Jr, and American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). ACC/AHA 2002 guideline update for exercise testing: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). Circulation. 2002 Oct 1;106(14):1883-92. DOI:10.1161/01.cir.0000034670.06526.15 |
- Alpert JS, Thygesen K, Antman E, and Bassand JP. Myocardial infarction redefined--a consensus document of The Joint European Society of Cardiology/American College of Cardiology Committee for the redefinition of myocardial infarction. J Am Coll Cardiol. 2000 Sep;36(3):959-69. DOI:10.1016/s0735-1097(00)00804-4 |
- Martin TN, Groenning BA, Murray HM, Steedman T, Foster JE, Elliot AT, Dargie HJ, Selvester RH, Pahlm O, and Wagner GS. ST-segment deviation analysis of the admission 12-lead electrocardiogram as an aid to early diagnosis of acute myocardial infarction with a cardiac magnetic resonance imaging gold standard. J Am Coll Cardiol. 2007 Sep 11;50(11):1021-8. DOI:10.1016/j.jacc.2007.04.090 |
- Austen WG, Edwards JE, Frye RL, Gensini GG, Gott VL, Griffith LS, McGoon DC, Murphy ML, and Roe BB. A reporting system on patients evaluated for coronary artery disease. Report of the Ad Hoc Committee for Grading of Coronary Artery Disease, Council on Cardiovascular Surgery, American Heart Association. Circulation. 1975 Apr;51(4 Suppl):5-40. DOI:10.1161/01.cir.51.4.5 |
- Novotný T, Sisáková M, Floriánová A, Toman O, Dohnalová I, Poloczek M, Kala P, Kyselová I, Dostálová L, Vít P, and Spinar J. [QT dynamicity in risk stratification in patients after myocardial infarction]. Vnitr Lek. 2007 Sep;53(9):964-7.
- Jensen BT, Abildstrom SZ, Larroude CE, Agner E, Torp-Pedersen C, Nyvad O, Ottesen M, Wachtell K, and Kanters JK. QT dynamics in risk stratification after myocardial infarction. Heart Rhythm. 2005 Apr;2(4):357-64. DOI:10.1016/j.hrthm.2004.12.028 |
- Chevalier P, Burri H, Adeleine P, Kirkorian G, Lopez M, Leizorovicz A, André-Fouët X, Chapon P, Rubel P, Touboul P, and Groupe d'Etude du Pronostic de l'Infarctus du Myocarde. QT dynamicity and sudden death after myocardial infarction: results of a long-term follow-up study. J Cardiovasc Electrophysiol. 2003 Mar;14(3):227-33. DOI:10.1046/j.1540-8167.2003.02431.x |
- Wung SF and Kahn DY. A quantitative evaluation of ST-segment changes on the 18-lead electrocardiogram during acute coronary occlusions. J Electrocardiol. 2006 Jul;39(3):275-81. DOI:10.1016/j.jelectrocard.2005.10.007 |
- Menown IB, Mackenzie G, and Adgey AA. Optimizing the initial 12-lead electrocardiographic diagnosis of acute myocardial infarction. Eur Heart J. 2000 Feb;21(4):275-83. DOI:10.1053/euhj.1999.1748 |
- Sgarbossa EB. Value of the ECG in suspected acute myocardial infarction with left bundle branch block. J Electrocardiol. 2000;33 Suppl:87-92. DOI:10.1054/jelc.2000.20324 |
External Links
A good introduction to [coronary angiography]